
The lateral collateral ligament (LCL) is a thin band of tissue on the lateral (or outside) part of the knee. The LCL connects the thighbone (femur) to one of the bones in the shin (the fibula) and helps provide stability to the knee joint.
An LCL injury occurs when there is a strain or tear to the ligament. LCL injuries are not as common as medial collateral ligament injuries – they make up only 2% of knee ligament injuries.
Symptoms of a LCL Injury
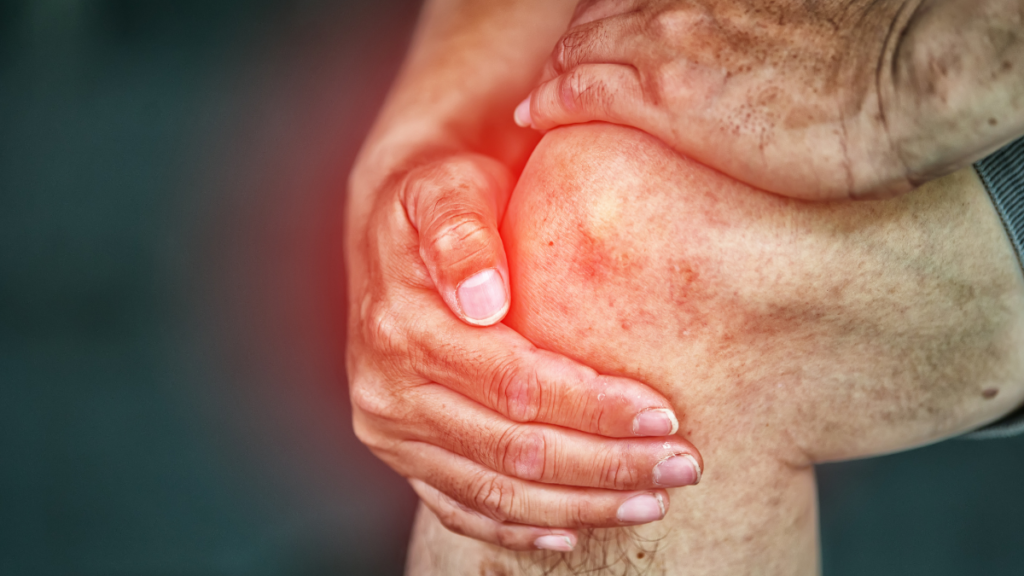
- Pain on the lateral (outside) part of the knee
- Swelling
- Decreased range of motion in knee
Other less common symptoms include numbness or tingling in the foot
Causes of a LCL Injury

- Direct blow to the inside of the knee
- Changing directions quickly or pivoting on one foot
- Landing awkwardly
- Hyperextending the knee
How to diagnose a LCL Injury
In most instances, a clinical examination with a physiotherapist or a sports and exercise physician will be able to identify signs and symptoms of a LCL injury. The clinician will ask a series of questions about what happened and conduct tests to determine the integrity of all of the ligaments, and other structures, in the knee.
An MRI scan can help identify a LCL tear as well as any other injury that can sometimes occur at the same time, such as bone bruising or meniscal (cartilage) injuries. An X-ray may be conducted to rule out an associated fracture (broken bone) that may have occurred on impact.
If you have any questions or concerns, please make sure you contact your local physiotherapist or sports and exercise physician.
Treatment options for a LCL Injury

In the acute phases (immediately after injury), it is important to follow the P.R.I.C.E.D principles:
- Protect your knee by off-loading and supporting the knee
- Rest your knee to avoid aggravating the injury
- Ice to reduce the swelling and pain
- Compression – you can use a compression bandage to reduce the swelling
- Elevate the knee as best you can to control swelling
- Diagnose – it is important you see a physiotherapist or medical professional so that they can assess and diagnose your knee injury
It is important to discuss treatment options with your physiotherapist, sports and exercise physician, or your GP. There are a number of factors that will influence your decisions about treatment including, but not limited, to:
- Your age
- Whether you are regularly involved in activities that involve a lot of twisting, jumping, change of direction etc
- Your goals
- Previous injuries
- What other responsibilities you have (e.g., work, family etc)
Non-Surgical Treatments
A specific and individualised knee rehabilitation program is considered the most effective non-surgical option to recover from a LCL injury. Physiotherapists are experts at designing rehabilitation programs to help you achieve your goals. The program is likely to focus on:
- Reducing pain and inflammation in the first instance
- Lower limb strengthening
- Balance and proprioception (body position awareness)
- Technique
- Overall conditioning program to help you return to your activities
For athletes, an additional focus on sport-specific agility and functional enhancement is also recommended.
There is good evidence that these types of programs can be very effective – it is really important you discuss whether non-surgical treatment is right for you with your physio or treating doctor.
Surgical Treatments
Surgery for a LCL injury is sometimes considered in more severe cases. It is important to discuss your treatment options with your physiotherapist, sports and exercise physician and/or the orthopaedic surgeon. An orthopaedic surgeon will explain the procedure and discuss what happens immediately after surgery.
Rehabilitation Post-Surgery
Following a LCL reconstruction, it is very important to focus on restoring motion, strength and endurance of the lower limb muscles to be able to return to regular activity. Each surgeon will have a slightly different post-operative protocol dependent on their surgical technique and preference. Please consult with your surgeon and treating physiotherapist to ensure you have a clear and comprehensive program that is right for you.
Final Tips
Isolated LCL injuries are not common – LCL injuries are often associated with other ligamentous or bony injuries. It is really important you see your physiotherapist or medical professional as soon as you can so they can accurately assess and diagnose the injury and ensure you receive the most appropriate treatment and management plan.
FAQs
How can I prepare for a physiotherapist appointment?
A physiotherapist will want to understand your area of concerns by discussing any factors that may contribute to your pain or immobility.
It is recommended that you note down any symptoms you are experiencing and when they began, your personal and family medical history, current medications, and any questions you might want to ask during your appointment.
What can I expect when seeing a physiotherapist?
A physiotherapist may conduct a physical examination of your area of concern, discuss your day-to-day activity and medical history, and prescribe a treatment plan for recovery.
When should I see a physiotherapist?
A physiotherapist can help you to reduce or manage pain and immobility throughout your body. If your concerns are impeding on your ability to participate in your regular activities, it may be time to see a physiotherapist.
The longer these concerns are left unattended, the harder they can be to treat down the track.
