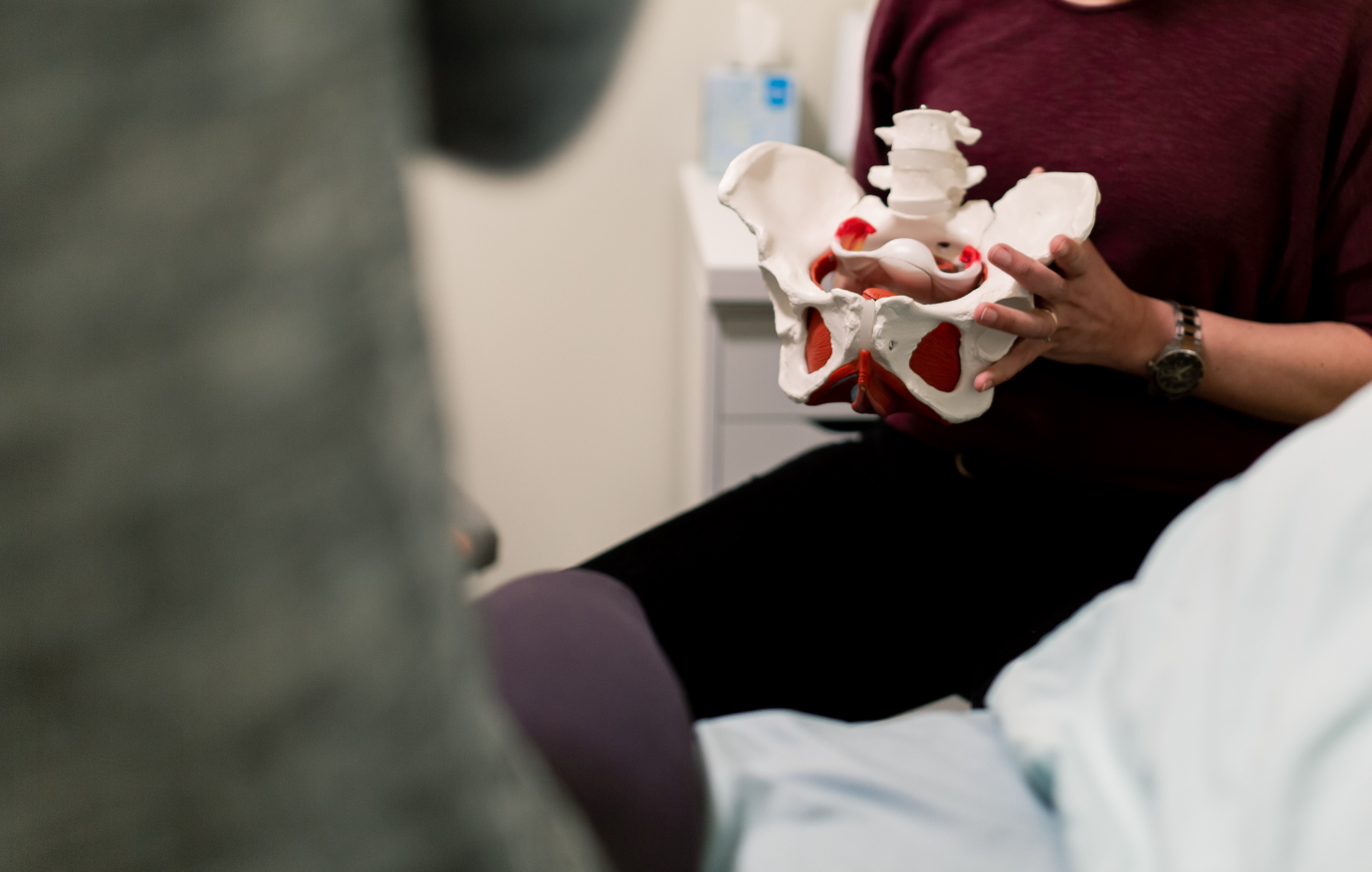
A woman’s life is typically marked by several unique life stages such as, menarche, pregnancy, childbirth and menopause. These stages are exclusive to women, and as such can provide specific challenges to a woman’s quality of life. One area of the body commonly impacted by these life stages, and the changes that come with them, is the pelvic floor. A group of small, but very important muscles, found at the base of the pelvis, the pelvic floor has a huge role to play throughout a woman’s life and is often overlooked. Pelvic floor dysfunction has been found to impact at least 25% of women at some stage of their life before they turn 80, and even doubles after this.
Pelvic floor dysfunction encompasses any symptom or sign that the activity or functioning of these muscles may be less than ideal. The pelvic floor muscles form a muscular “sling” at the base of our pelvis and work to support and hold in our pelvic organs, provide bladder and bowel continence (ability to control movements), are involved in healthy sexual function and childbirth. It is easy to see how, in any disorder or disease relating to the pelvis or it’s associated organs, normal healthy functioning of the pelvic floor can be easily compromised.
Common issues that may cause someone concern about how their pelvic floor is functioning can include:
- Bladder disorders such as involuntary leakage of urine (stress or urge incontinence) and even overactive bladder syndrome (dysfunction of bladder filling and emptying)
- Bowel disorders such as involuntary leakage of faeces (poo) or flatus (wind), termed faecal incontinence, and even concerns with stool type such as, chronic constipation or diarrhoea
- Loss of support of pelvic organs (pelvic organ prolapse)
- Pelvic pain disorders and sexual dysfunction
- Pregnancy and childbirth specific issues or injuries
Issues associated with pelvic floor dysfunction can be highly sensitive, often thought of as “taboo”, and difficult for the individual experiencing them to discuss. These conditions can be complex and there is often a broad range of overlapping medical issues associated with pelvic floor dysfunction, requiring medical assessment and management with a multidisciplinary team. In all this complexity, the role of the pelvic floor muscles can be forgotten, despite the strong evidence that exists to support pelvic floor physiotherapy in the management of a lot of these conditions.
A women’s pelvic health trained physiotherapist is key in the multi-disciplinary management of someone with pelvic floor concerns. They are specially trained to help women manage pelvic floor dysfunction across the lifespan, with strong evidence supporting their involvement in management of all pelvic floor conditions. A women’s health physiotherapist will perform a highly individualised assessment and can work with you to help manage your pelvic floor concerns in a variety of ways, such as:
- Postural, ergonomic and biomechanical modifications related to symptom onset or aggravation
- Management of associated or contributing musculoskeletal conditions
- Prescription of appropriate pelvic floor exercises, stretches or even relaxation
- Help with healthy bladder and bowel habits, in order to avoid conditions such as chronic constipation which is known to aggravate pelvic floor dysfunction
- Pain management techniques and treatments for chronic pelvic pain conditions and to help support normal, healthy sexual function
- Prescription of supportive devices such as pessaries for pelvic organ prolapse (where appropriate)
- Lifestyle advice to support pelvic health such as general exercise prescription and weight management
- Pregnancy management, pain relief options and positioning for labour and childbirth, postnatal assessment and treatment and longer-term guidance for safe return to exercise
If you have any concerns regarding your pelvic floor health, or have been advised to see a physiotherapist for your symptoms, please reach out to your local clinic to see how one of our Women’s Health Physiotherapists could help you today.
References
Berghmans, B. (2018). Physiotherapy for pelvic pain and female sexual dysfunction: An untapped source. International Urogynecology Journal. 29, 631-638.
Grimes WR, Stratton M. (2022). Pelvic Floor Dysfunction. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
Hagen, S. & Stark, D. (2011). Conservative prevention and management of pelvic organ prolapse in women. Cochrane Database of Systematic Reviews. 12.
Hartmann, D. & Sarton, J. (2014). Chronic pelvic floor dysfunction. Best Practice & Research in Clinical Obstetrics and Gynaecology. 28, 977-990.
Hay-Smith, E. J. C., Herderschee, R., Dumoulin, C. & Herbison, G. P. (2011). Comparisons of approaches to pelvic floor muscle training for urinary incontinence in women. Cochrane Database of Systematic Reviews. 12.
Herschorn, S. (2004). Female pelvic floor anatomy: The pelvic floor, supporting structures and pelvic organs. Reviews in Urology, 6 (5), S2-S10.
International Organisation of Physical Therapists in Women’s Health 2013 Scope of Practice (PDF), IOPTPWH.
Kahyaoglu, S.H. and Balkani, K.P. (2016). Effect of pelvic floor muscle exercise on pelvic floor muscle activity during pregnancy and the postpartum period. Neurology and Urodynamics. 35 (3), 417-422.
Kenne, K.A., Wendt, L. & Brooks Jackson, J. (2022). Prevalence of pelvic floor disorders in adult women being seen in a primary care setting and associated risk factors. Scientific Reports. 12, 9878.
Sung, V. W. & Hampton, B. S. (2009). Epidemiology of pelvic floor dysfunction. Obstetrics & Gynaecology Clinics. 36 (3), 421 – 443.
Weiss, P. M., Rich, J., & Swisher, E. (2012). Pelvic floor spasm: The missing link in chronic pelvic pain. Contemporary OB/GYN.
Our Community Partners