Almost everyone has heard of sciatica. But when we talk about this condition, it can be a bit unclear what it actually is.
The term is often used quite loosely, for example to describe different types of leg pain that aren’t necessarily connected to the sciatic nerve.
There are also some common myths around sciatica, especially regarding diagnosis and treatment.
Here’s an outline of the symptoms and treatments for sciatica, plus a little myth-busting!
What is sciatica?
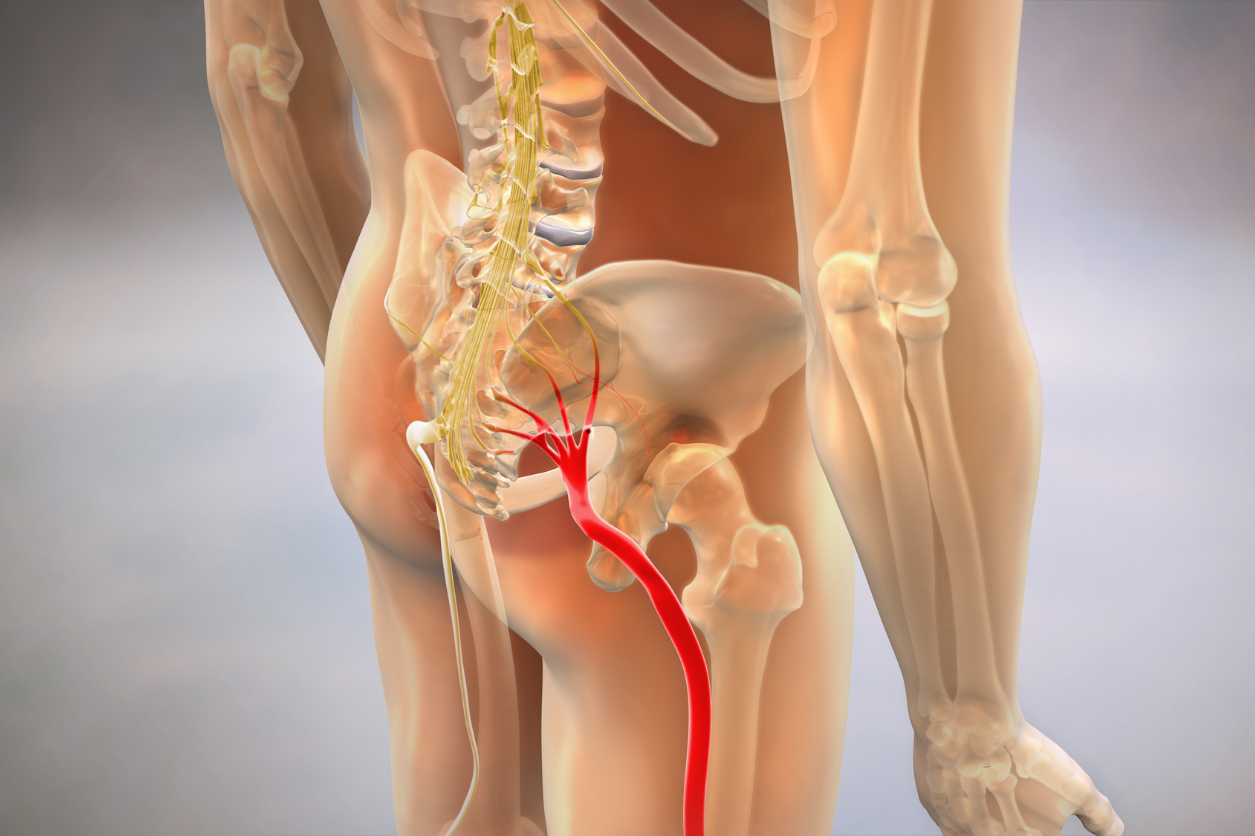
The term ‘sciatica’ refers to nerve pain in the leg caused by irritation to or pressure on the sciatic nerve. This is a large nerve that starts in the lower back and passes through the buttock down the back of the leg.
While sciatica is thought of as a health condition, it’s really more a symptom than a diagnosis in itself – it describes the pain the sufferer experiences. There can be a number of causes of sciatica. The most common is a herniated disc in the lower back. Other less common causes include stenosis (narrowing of the opening the nerve travels through) and certain types of spinal disorder.
What are the symptoms of sciatica?
The signs of sciatica include:
- Dominant leg pain – that is, pain that is stronger than any back pain being experienced.
- Increased leg pain with coughing, sneezing and/or deep breaths.
- Tingling, numbness or weakness in the affected leg. These sensations may also affect leg movement.
- Sharp or shooting pain felt deep in the buttock.
Symptoms of sciatica typically last a few weeks, although they could be longer in some people. Recurring flare-ups may also sometimes occur.
How is sciatica diagnosed and treated?
Diagnosis involves asking the patient about their symptoms, doing a physical exam (e.g. testing for loss of muscle strength) and ruling out other serious conditions that could be causing the pain.
Treatment may include pain medications, physical therapies, physical activities (i.e. exercises) or surgery. Treatment is tailored to the individual – what works for one person may not for another.
There is also limited evidence for any single type of remedy for all sciatica conditions.
What are some of the common myths?
Myth 1 – the diagnosis should include a scan
Imaging scans are generally not very useful for diagnosing sciatica. This is because they do not appear to provide any information that proves useful for managing the condition. Imaging can also have a negative psychological effect on patients – even leading to worsening or prolonging of their pain.
Scans may be recommended in some cases however – such as where another serious condition is suspected (e.g. a fracture).
Myth 2 – you should rest in bed to recover
The traditional ‘bed rest’ approach is no longer generally recommended for sciatica. Studies show prolonged bed rest usually makes little or no difference for recovery from the condition.
These days, people with sciatica are more often encouraged to stay active. Gentle exercises may also be useful in some cases – although no specific set of exercises that help across the board has been identified.
An exercise program is likely to be more effective where it is tailored to the individual. It may include exercises for improving strength, nerve mobilisation or motor control. Most people are more likely to continue with an exercise program if they enjoy it, or it gives them relief!
Myth 3 – you need strong pain medication to manage sciatica
The types of prescribed medication used to treat sciatica include corticosteroids, anti-depressants, anticonvulsants, anti-inflammatories and opioid analgesics.
However, several trials show that these types of medications are mostly no more effective than placebo – making their usefulness very limited.
These medications can also have serious side-effects, which could make them not worthwhile even where mild pain relief is provided.
Myth 4 – surgery is needed for sciatica
In most cases of sciatica, surgery isn’t required. However, where the pain doesn’t subside with normal treatment, lower back surgery may be a consideration.
That said, results from surgery have been shown to be relatively modest.
Call us for expert help on sciatica
Are you experiencing lower back or leg pain and are concerned it could be sciatica? If so, book a time to see one of our physiotherapists.
References
[1] Physiotherapy management of sciatica
[2] Advice to rest in bed versus advice to stay active for acute low-back pain and sciatica
Our Community Partners